Spring is here: longer days, warmer air, and an irresistible force pull us outdoors to enjoy the sunlight after the dark winter (unless you live in California, where it is sunny also in the winter!)
The sun is the single greatest source of radiation we encounter in everyday life.
Our relationship with sunlight is two-sided. On one hand, it lifts our mood and helps our skin cells to make Vitamin D, which is fundamental for the absorbption of calcium and phosphorus, making for stronger bones and teeth1. Ultraviolet (UV) rays play a fundamental part in Vitamin D metabolism by converting a precursor molecule (7-dehydrocholesterol) into pre-vitamin D3, which then rearranges into Vitamin D3. On the other side, UV radiation (Figure 1) is classified as a human carcinogen by the International Agency for Research on Cancer and is responsible for the vast majority of skin cancers, accounting for approximately 90% of non-melanoma skin cancers (NMSC) and an estimated 65%- 90% of melanomas2, 3.
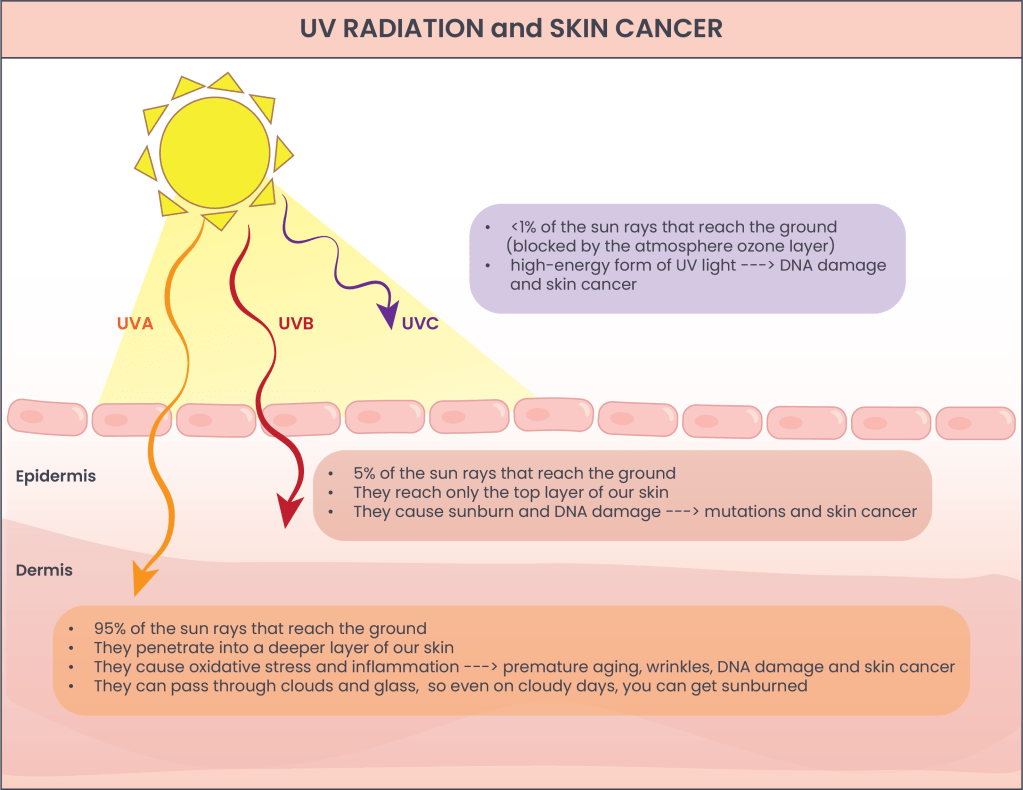
Figure 1: The sun emits different types of radiation, including visible light or sunlight (that we can see), infrared radiation (that we can feel as heat), and UV radiation, that can’t be seen or felt. There are three types of UV radiation, based on wavelength: UVA, UVB, and UVC. Each behaves differently and carries a different risk profile for the skin.
UV radiation and skin cancer
Skin cancer is the most common cancer worldwide. In the United States alone, more skin cancers are diagnosed each year than all other cancers combined4. The good news is that, since we know the risk factors, it is also one of the most preventable. UV radiation damages the DNA of skin cells – triggering mutations that, if not repaired, can lead to cancer development. Prolonged and unprotected exposure to all sources of UV rays, whether it’s sunlight or tanning devices, is a major risk factor for all types of skin cancer, primarily:
- NMSC, which comprise basal and squamous cell skin cancers: mostly benign, they originate from cell in the top layer of the skin;
- melanoma: the most dangerous form, originating from melanocytes. These cells produce the brown pigment called melanin and also form moles5. Melanin protects the skin from some of the harmful effects of the sun – but alone is not enough to protect us from cancer!
Risk factors include cumulative lifetime UV exposure, history of sunburns (particularly in childhood), use of tanning beds (classified as carcinogens), fair skin, a family history of skin cancer, and a large number of moles. However, skin cancer can affect people of all skin tones, and protection matters for everyone.
Sunscreen: your daily shield
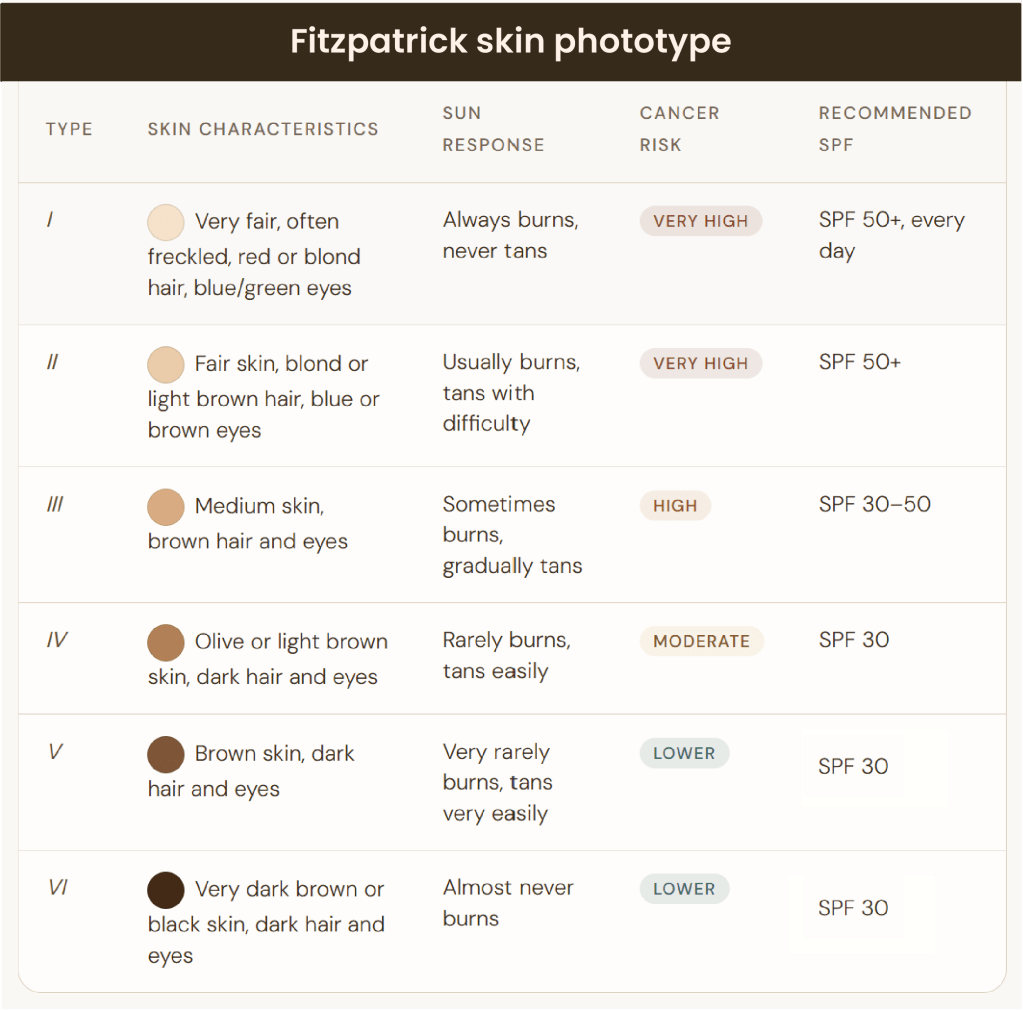

Table 1: The Fitzpatrick phototype classification, developed by dermatologist Thomas B. Fitzpatrick in 1975, is still referenced to determine skin reaction to UV radiation based on melanin levels and to guide sun protection recommendations.
Sunscreen is one of the most evidence-based tools for skin cancer prevention. Regular daily use has been shown to reduce the incidence of squamous cell carcinoma by approximately 40% and melanoma by 50%, according to long-term studies6. But choosing it and applying it correctly makes all the difference. There are two main categories of sunscreens:
- Chemical-based sunscreens absorb UV rays into the skin and deactivate them by turning them into heat. Chemical sunscreens include ingredients like avobenzone and octocrylene, are generally easy to apply, but can cause reactions and allergies so are less indicated for sensitive skin.
- Mineral-based sunscreens act like a physical barrier, by deflecting and scattering UV rays. They contain ingredients like zinc oxide and/or titanium dioxide. Generally well-tolerated by sensitive skin and recommended for children. May be harder to rub in and leave a white cast, though newer formulations minimize this.
Sunscreen can also have a combination of both physical and chemical blockers. The Center for Disease Control and Prevention (CDC) recommends using broad spectrum sunscreen against both UVA and UVB with suitable Sun Protection Factor (SPF)7. SPF measures a sunscreen’s ability to protect skin against UVB. The SPF number tells you how much longer someone can stay in the sun without burning compared to unprotected skin. For example, SPF 30 means the skin is theoretically protected 30 times longer than without sunscreen. Not everyone’s skin responds the same way to the sun and recommendation of which SFP to use depends on your skin tone (Table 1). In general, it is recommended to use at least SPF 30 for all skin types.
How is the protection against UVA indicated on the sunscreen instead? It changes from country to country. While in the USA the term “broad spectrum” is used, in Europe a UVA circled logo is present, and more general international guidelines use the PA+ system ( PA+ “some protection” to PA++++ “extremely high protection”).
Also the correct application matters: the recipe for a perfect protection is to apply is 2 mg/cm2 – which translating into Imperial units it roughly corresponds to 1 tablespoon (tbs) for face and neck, 1 tbs for each arm, 2 tbs for the torso and 2 tbs for each leg (for an average adult). Sunscreen should be reapplied every 2 hours, and after sweating or swimming to maintain protection – even when using a waterproof product.
One question now may arise: can we still get enough Vitamin D even when protecting our skin with sunscreen? The answer we have so far from research is yes, as there is no evidence of Vitamin D deficiency caused by sunscreen use8. Besides, you can always supplement Vitamin D intake, but you can’t take back the DNA damage caused by UV radiation!
Protecting skin and beyond: a practical guide
Sun protection is most effective when it combines multiple strategies. No single measure is sufficient on its own, but together they dramatically reduce UV exposure. Most Health Institutions recommend to:
- Seek shade especially between 10 am and 4 pm, when UV radiation is most intense – the “shadow rule”9 is a good guide: if your shadow is shorter than you are, the sun is at its strongest9.
- Protect your body with sunscreen, clothes and hats.
- Don’t forget about your eyes! UV exposure affects the eyes and can contribute to cataracts and eye cancers. Make sure your sunglasses also provide UVA/UVB-protection10.
- Avoid tanning beds entirely. They emit UVA and have no safe threshold for use.
- Be especially mindful near water, sand, and snow – these surfaces reflect UV radiation and significantly increase exposure.
- Remember that UVA rays can penetrate clouds, so don’t be fooled by cloudy days.
Sun exposure is not inherently dangerous – in fact, moderate exposure is beneficial. The risk lies in excess, and in the nature of the exposure. Understanding how solar radiation affects our body – especially our skin – is important to safely enjoy the sun, year after year.
| A Note on Radiation and Imaging TestsThe sun is not the only source of radiation whose benefits and risks are worth weighing. Medical imaging tests that use radiation such as X-rays, CT scans, and PET scans can also contribute to our lifetime radiation exposure. According to the American Cancer Society, it’s important to put this risk into perspective. The low doses involved in imaging tests may slightly increase cancer risk, but experts consider this increase to be very small, and the diagnostic benefit generally outweighs the risk. You can find more information about radiation risk from imaging tests here. |
- Raymond-Lezman JR, Riskin SI. Benefits and Risks of Sun Exposure to Maintain Adequate Vitamin D Levels. Cureus. 2023 May 5;15(5):e38578. doi: 10.7759/cureus.38578. PMID: 37284402; PMCID: PMC10239563. ↩︎
- Kim Y, He YY. Ultraviolet radiation-induced non-melanoma skin cancer: Regulation of DNA damage repair and inflammation. Genes Dis. 2014 Dec 1;1(2):188-198. doi: 10.1016/j.gendis.2014.08.005. PMID: 25642450; PMCID: PMC4307792. ↩︎
- Centers for Disease Control and Prevention (April 26, 2002). Guidelines for School Programs To Prevent Skin Cancer cdc.gov Retrieved April 12th 2026 from https://www.cdc.gov/mmwr/pdf/rr/rr5104.pdf ↩︎
- American Academy of Dermatology Association (March 2nd 2026) Skin cancer. aad.org. Retrieved April 5th 2026 from https://www.aad.org/media/stats-skin-cancer. ↩︎
- American Cancer Society. (26 June 2024) UV (Ultraviolet) Radiation and Cancer Risk. Cancer.org. Retrieved April 5th 2026 from https://www.cancer.org/cancer/risk-prevention/sun-and-uv/uv-radiation.html. ↩︎
- Sander M, Sander M, Burbidge T, Beecker J. The efficacy and safety of sunscreen use for the prevention of skin cancer. CMAJ. 2020 Dec 14;192(50):E1802-E1808. doi: 10.1503/cmaj.201085. PMID: 33318091; PMCID: PMC7759112. ↩︎
- The University of Texas MD Anderson Cancer Center ( 18 June 2024) How does sunscreen work? Understanding UV protection. mdanderson.org Retrieved April 6th 2026 from https://www.mdanderson.org/cancerwise/how-does-sunscreen-work.h00-159698334.html. ↩︎
- Neale RE, Khan SR, Lucas RM, Waterhouse M, Whiteman DC, Olsen CM. The effect of sunscreen on vitamin D: a review. Br J Dermatol. 2019 Nov;181(5):907-915. doi: 10.1111/bjd.17980. Epub 2019 Jul 9. PMID: 30945275. ↩︎
- United States Environment Protection Agency. (22 January 2026) UV Index Scale. epa.gov Retrieved April 6th 2026 from https://www.epa.gov/sunsafety/uv-index-scale-0. ↩︎
- The University of Texas MD Anderson Cancer Center( 31 July 2024) 9 things to know about sunglasses, eye protection and cancer mdanderson.org Retrieved April 6th 2026 from https://www.mdanderson.org/cancerwise/9-things-to-know-about-sunglasses–eye-protection-and-cancer.h00-159699123.html#:~:text=UV%20exposure%20can%20cause:%20*%20**Basal%20cell,eyeball%22%2C%20this%20is%20a%20very%20painful%20condition. ↩︎
© 2025 WithinOncology. All rights reserved.
This article, including all text, tables, and figures, is the intellectual property of WithinOncology and its contributors. Unauthorized reproduction, distribution, or use of any content without explicit written permission is strictly prohibited. For inquiries, please contact us via the contact form.


Leave a comment