If T-cells are the conductors of our immune system, they bring to life the music composed by B-cells. Without the composer, great works would never be remembered. Their lives and capabilities are a culmination of countless moments – as for all of us – yet in precious few they wrote the music they will be remembered for. We previously took a broader look at how our immune system works. Here, we will focus on early lives of B-cells, and how they create their magnum opus: their unique antibodies. They are nomadic cells, traveling far and wide to put their skills to the test in the hopes that theirs will be a melody for the ages.
The two B-cell varieties
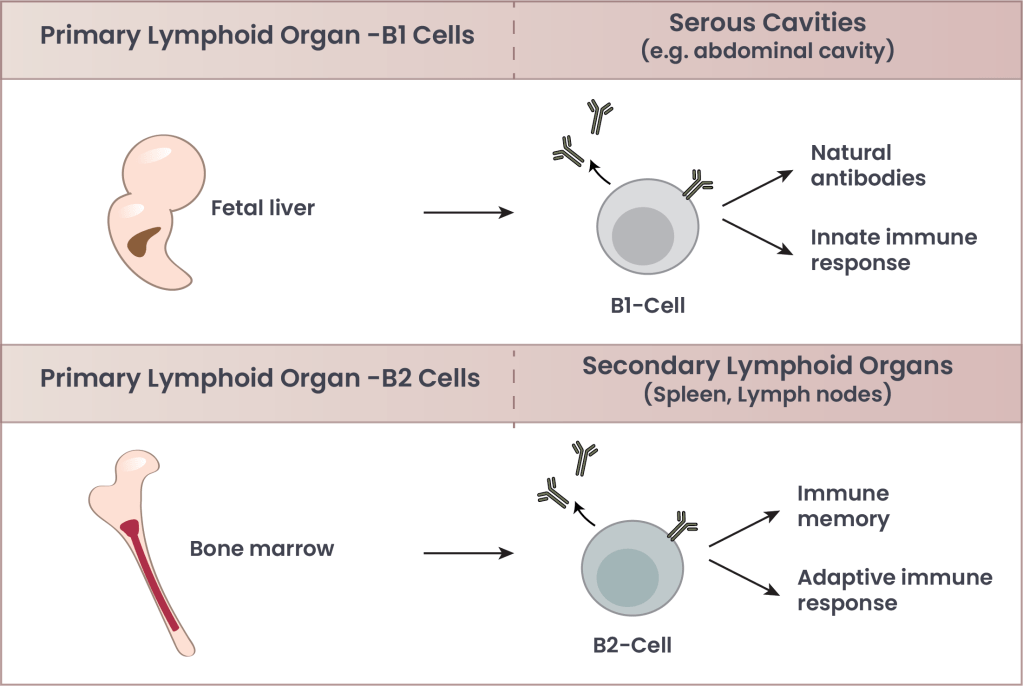
Figure 1. Key differences between B1 and B2 cells. B1 cells and the natural antibodies they produce are determined early in development from lymphoid progenitor cells. Once we are developed, they migrate to cavities throughout our body, prepared to release natural antibodies that participate in the innate immune system, clearing out dead, dying, or unhealthy cells, among other roles. B2 cells are produced in our bone marrow, and then mature fully in the spleen and lymph nodes. They participate in the adaptive immune response by learning from pathogenic threats, and producing increasingly effective antibodies that protect from future encounters with known pathogens.
The early years of our protagonist’s life set the stage for their later years. Early in development, lymphoid cells, the progenitors for almost all immune cells, become B1 or B2 cells depending on where they are in the body and what they were exposed to, in a process that is still poorly understood. B1 cells don’t “learn” as much as B2 cells, and instead produce a host of natural antibodies that recognize common antigens, but also support health in pathogen-independent ways. For example, some recognize the stalk region of hemagglutinin of the influenza A virus, while others recognize dying or sick cells that need to be cleared out, or modulate immune responses. These cells reside throughout cavities in our body and play important roles in the innate immune system1. When we think of our immune memory, or the adaptive immune system, we are thinking of B2 cells (Figure 1). For this reason, we will simply refer to B2 cells as “B-cells.”
How B-cells develop and test their melodies
New B-cells develop throughout our adult lives. Each B-cell matures in two stages. After forming in the bone marrow, they migrate to the spleen where they begin the first stage in our bone marrow, when each B-cell creates its melody: its own unique B-cell receptor (BCR). Two genes are used to create these receptors, immunoglobulin heavy, and immunoglobulin light. B-Cells don’t know what antigens they will need to detect later on – composers are brilliant, but they can’t predict the future – so they prepare for as many scenarios as possible. Preparation is a numbers game: purposeful, semi-random mutation of BCR genes and shuffling parts of genes around results in up to 50 trillion unique BCRs2. This process is like changing and shuffling parts of music around until one combination sticks out as a potential winner. While each individual B-cell and its BCR can only detect one antigen, B-cells are prepared for the unexpected by producing countless cells with unique BCRs. This unique melody lays the foundation for future success and improvement. If all goes well, the BCR is eventually turned into antibodies.
Once their BCR is fully expressed, B-cells enter their second phase of maturation, the “transitional” phase, and leave the bone marrow to see if their melodies are any good – testing their BCRs and antibodies against antigens. Transitional B-cells migrate to secondary lymphoid organs (like the spleen and lymph nodes) that act like antigen checkpoints, collecting potentially dangerous molecules from throughout the body. B-cells patrol these organs, testing whether their unique receptor matches any of the collected antigens. If they don’t sense an antigen, they eventually move out of the organ and continue their surveillance elsewhere. However rare, a BCR recognizing an antigen signifies success of the B-cell, and it starts to improve on its melody in preparation for the final piece.
Capitalizing on success: responses to antigen-BCR interactions
Encountering an antigen activates the B-cell – it knows it’s made it big. Activation entails a series of responses starting with a prolonged stay in the current organ of residence. T-cells may also boost the B-cell response if antigen signals are weak (Figure 2). Responses are modulated by other molecules, called co-receptors. To give an example, CD19 is a major stimulatory co-receptor that sits on the cell close to the BCR. It recruits signaling molecules to the internal part of the BCR to amplify the response. It also modulates B-cell activation threshold. This threshold exists to prevent look-a-like yet benign antigens from triggering a response – this is part of autoimmunity prevention2. One outcome of B-cell activation is internalization of the antigen, in which the antigen is brought inside the cell. The antigen is then chopped up into pieces, and presented externally like a red flag to activate surrounding T-cells3. Activated B-cells are the precious few whose random mutations resulted in a BCR corresponding to an antigen – to capitalize on this good fortune, they first proliferate significantly. During these rounds of cell growth, their antibodies mutate further to generate an even wider variety in a process called “class switch recombination”. Several different types can ultimately be made (IgM, IgG, IgA, IgE, IgD), all targeting the same antigen but serving a different purpose (Table 1) – imagine the same melody being played in rock, classical, pop, or jazz styles.
| Ig Type | Function |
|---|---|
| IgM | Produced in early immune responses to pathogens |
| IgG | Produced in later immune response to pathogens |
| IgA | Main antibody produced in saliva, tears, etc. |
| IgE | Protects against parasites, causes allergic reactions |
| IgD | Unknown function |
Table 1. The five types of immunoglobulin4.
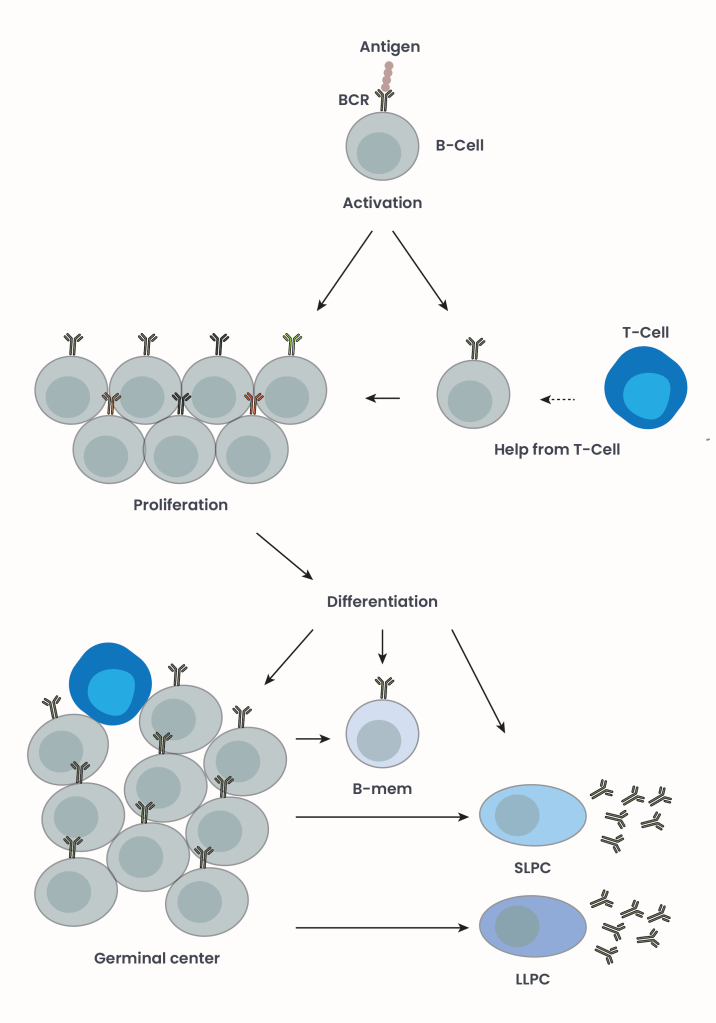
Figure 2. B-cell activation. A BCR encountering an antigen leads to B-cell activation. If the activation signal is weak, T-cells may assist. Activated B-cells multiply while undergoing class switch recombination, becoming mature naive B-cells. These then differentiate further into either germinal centers, B-memory cells (B-mem), or short-lived plasma cells (SLPCs). Germinal centers form with the assistance of T-cells, and can differentiate into B-mem, SLPCs, and long-lived plasma cells (LLPCs). B-mem cells persist long-term to store immune memory, SLPCs are short lived and produce antibodies early during immune responses, and LLPCs persist long term and continue to produce antibodies that constantly surveil the body for target antigens. Picture adapted from Cyster and Allen, 20195.
Cells at this stage are called “mature naive B-cells,” and can differentiate into one of four possible cell types2 (Figure 2):
- B memory cells (B-mem): These can be generated from either mature naive B-cells or germinal centers, similar to SLPCs. Along with LLPCs, they make the basis for immune memory. They can enter dormancy, a hibernation-like state, in which they preserve immunological memory over extended periods, standing ready to mount a rapid response when they re-encounter the antigen that activated them. They can become germinal centers or plasma cells upon activation.
- Germinal centers: This is a key state in the journey of B-cells. Directing T-cells are required for this process. Germinal centers induce further proliferation. Additionally, another round of antibody gene mutation leads to improved antibodies, capable of more strongly binding the target antigen. Stronger antibody-antigen interactions lead to stronger B-cell activation. These leveled-up cells are “selected for”, meaning they are enriched in the population relative to cells with weaker antibodies. B-cells can then further differentiate into plasma or memory cells.
- Short-lived plasma cells (SLPCs): These can be generated directly from mature naive B-cells, or from germinal centers. They are produced early during proliferation to produce antibodies, and don’t stick around for long.
- Long-lived plasma cells (LLPCs): These are produced by germinal centers. LLPCs persist and continually produce antibodies.
Closing words
Our remarkable immune system consists of equally remarkable cells. They didn’t start out that way, however. The journey that B-cells set out on is long, and wrought with failure: for each individual antigen that can be detected, a single B-cell is made, yet a miniscule fraction ends up recognizing an antigen. It’s thanks to these lucky few B-cells that we gain protection from pathogens, and even cancer. Our bodies continue to write the musical scores that make up our immune memory throughout our lives, and we are now learning how to boost and guide that process. Understanding new aspects of B-cell biology, uncovered by ongoing research, sheds light on autoimmune diseases, and fuels treatments including novel cancer therapies.
- Mattos, M. S., Vandendriessche, S., Waisman, A. & Marques, P. E. The immunology of B-1 cells: from development to aging. Immun. Ageing 21, 54 (2024). ↩︎
- Gómez-Manríquez, J. et al. B cell development: transcriptional regulation and immunological mechanisms in homeostasis. Front. Immunol. 16, 1593338 (2025). ↩︎
- Rastogi, I. et al. Role of B cells as antigen presenting cells. Front. Immunol. 13, 954936 (2022). ↩︎
- Luzzatto, L., Ally, M. & Notaro, R. Glucose-6-phosphate dehydrogenase deficiency. Blood 136, 1225–1240 (2020). ↩︎
- Cyster, J. G. & Allen, C. D. C. B Cell Responses: Cell Interaction Dynamics and Decisions. Cell 177, 524–540 (2019). ↩︎
© 2025 WithinOncology. All rights reserved.
This article, including all text, tables, and figures, is the intellectual property of WithinOncology and its contributors. Unauthorized reproduction, distribution, or use of any content without explicit written permission is strictly prohibited. For inquiries, please contact us via the contact form.


Leave a comment